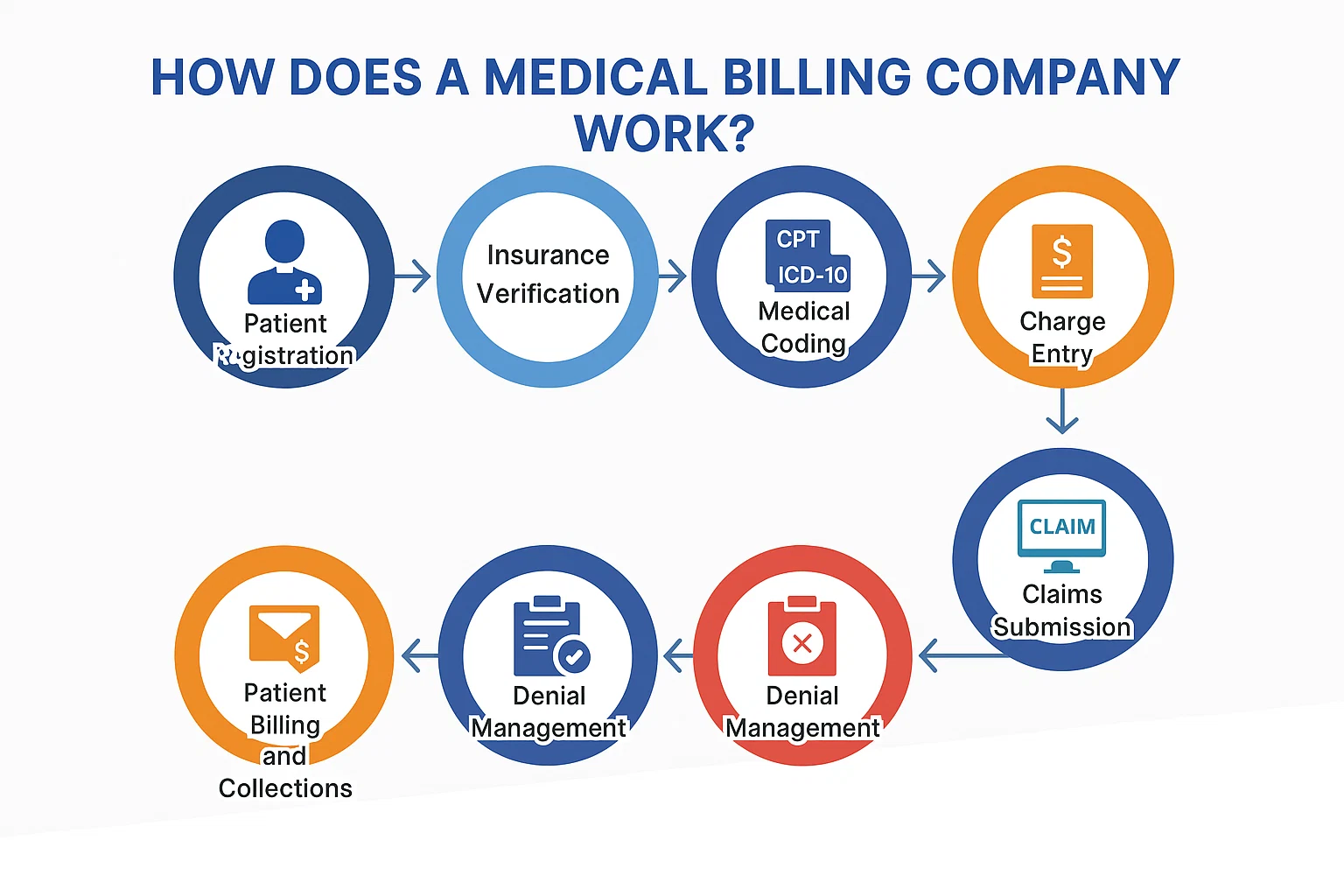
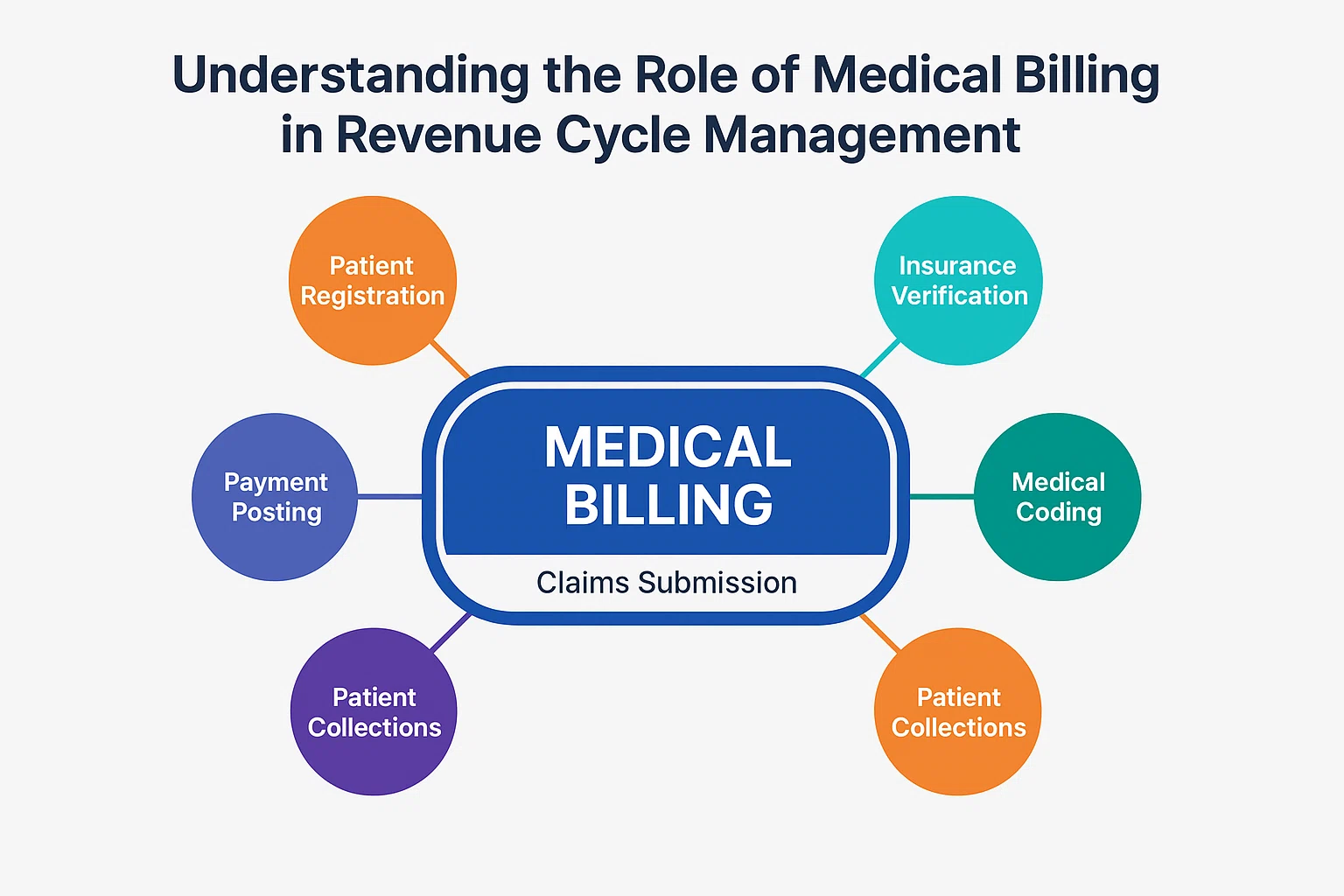
In the intricate world of healthcare, ensuring accurate and timely reimbursement is paramount. Medical billing companies are crucial in bridging the gap between healthcare providers and insurance payers. This article delves into the step-by-step processes that underpin the operations of a medical billing company like Laftic, highlighting how each phase contributes to efficient revenue cycle management.
1. Patient Registration
The journey begins with patient registration. Accurate collection of demographic details—such as full name, date of birth, address, and insurance information—is essential. This foundational data ensures that subsequent billing processes are based on correct and complete information, minimising the risk of claim denials due to inaccuracies.Bryant & Stratton College
2. Insurance Verification
Once registration is complete, verifying the patient’s insurance coverage is the next critical step. This involves confirming the validity of the insurance policy, understanding the scope of coverage, identifying co-pays, deductibles, and any pre-authorisation requirements. Effective insurance verification ensures that services rendered are billable and reduces the likelihood of claim rejections.
3. Medical Coding
Medical coding translates healthcare diagnoses, procedures, and services into standardised codes using systems like ICD-10 and CPT. Accurate coding is vital, as it directly impacts reimbursement. Certified medical coders analyse clinical documentation to assign appropriate codes, ensuring compliance with regulations and facilitating smooth claim processing.
4. Charge Entry
In this phase, the coded information is entered into the billing system, assigning monetary values to each service provided. Charge entry must align with the coding to ensure that claims reflect the actual services rendered. Precision in this step is crucial to prevent discrepancies that could lead to claim denials or underpayments.AIHCP
5. Claims Submission
After charge entry, claims are prepared and submitted to insurance companies. This process often involves electronic submission through clearinghouses, which act as intermediaries to detect errors and ensure compliance with payer-specific requirements. Submitting “clean claims”—those free from errors—enhances the likelihood of prompt reimbursement.
6. Payment Posting
Upon receiving payments from insurers, the billing company posts these payments to the patient’s account. This step involves reconciling the received amount with the billed charges, noting any discrepancies, adjustments, or denials. Accurate payment posting provides a clear financial picture and aids in identifying outstanding balances.
7. Denial Management
Not all claims are accepted on the first submission. Denial management involves analysing rejected or denied claims to determine the reasons, be it coding errors, missing information, or non-covered services. The billing company then rectifies these issues and resubmits the claims, ensuring that providers receive due compensation.
8. Patient Billing and Collections
After insurance payments are accounted for, any remaining balances are billed to the patient. Clear and concise billing statements are sent, detailing the services provided, insurance contributions, and the patient’s financial responsibility. Effective communication and follow-up strategies are employed to facilitate timely collections.
9. Reporting and Analytics
Medical billing companies generate comprehensive reports that provide insights into the financial health of healthcare practices. These reports cover metrics like claim acceptance rates, average reimbursement times, and outstanding balances. Such analytics empower providers to make informed decisions and optimise their revenue cycles.
10. Compliance and Continuous Improvement
Staying abreast of regulatory changes is imperative. Medical billing companies ensure compliance with laws like HIPAA and adapt to updates in coding standards. Continuous training and process evaluations are conducted to enhance efficiency, reduce errors, and maintain the highest standards of service.
Conclusion
The operations of a medical billing company encompass a series of meticulous steps, each integral to the seamless management of healthcare revenue cycles. By entrusting these processes to experts like Laftic, healthcare providers can focus on delivering quality patient care, confident that their billing and reimbursement systems are in capable hands.