Revenue Cycle Management (RCM) is the backbone of a healthcare organization’s financial health. Among its many moving parts, medical billing plays a central role in ensuring that providers are properly reimbursed for the services they deliver. This article breaks down the RCM process and highlights how accurate, timely medical billing supports sustainable operations, improved cash flow, and fewer denials.
1. What is Revenue Cycle Management (RCM)?
Revenue Cycle Management is the financial process that healthcare organizations use to track patient care episodes from registration and appointment scheduling to the final payment of a balance. It integrates clinical and administrative functions such as billing, claims processing, coding, and revenue collection into one cohesive system.
An effective RCM system is critical for the profitability and operational efficiency of any healthcare provider. It reduces delays, limits denied claims, and ultimately ensures that the provider gets paid for services rendered.
2. The Core Stages of Revenue Cycle Management
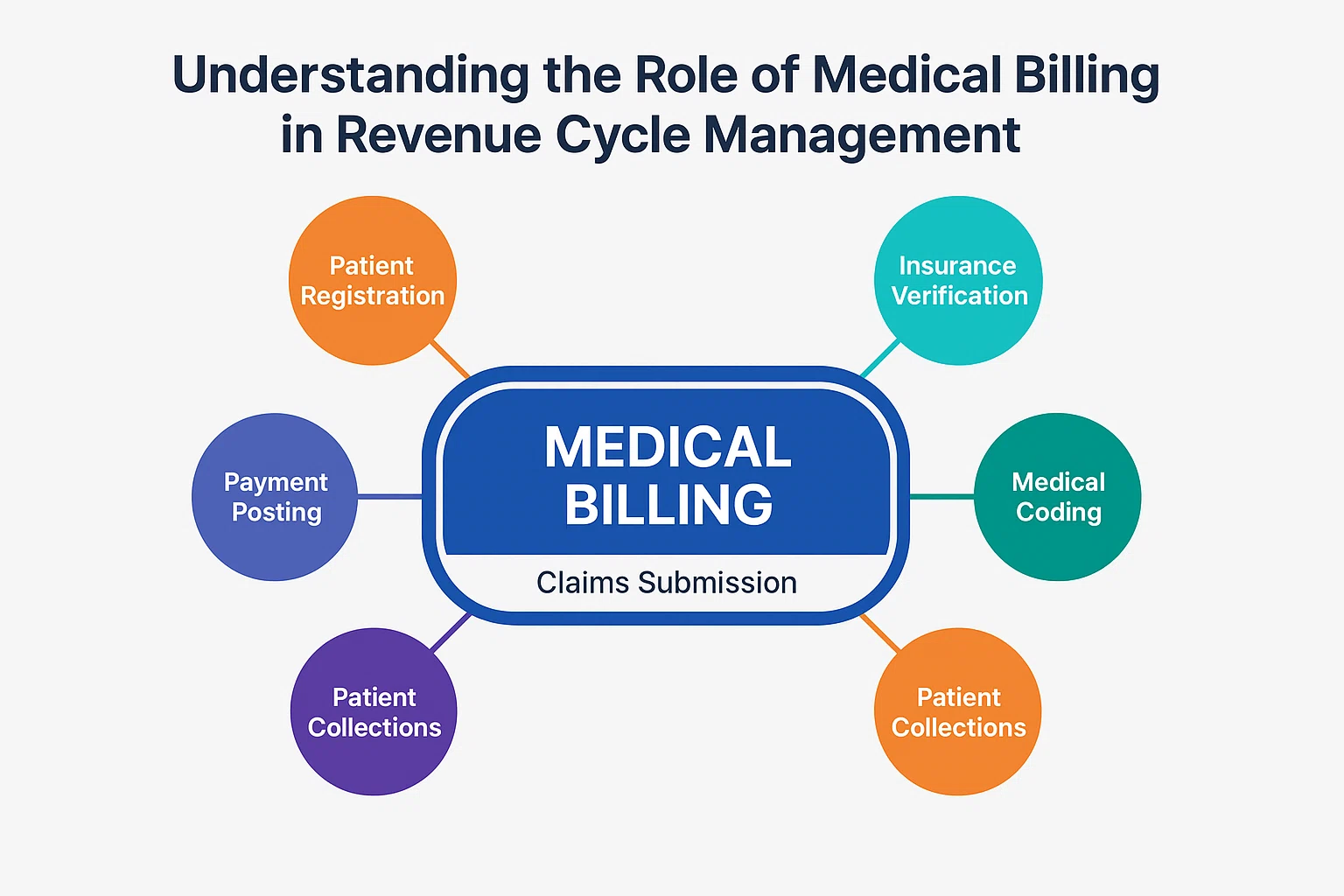
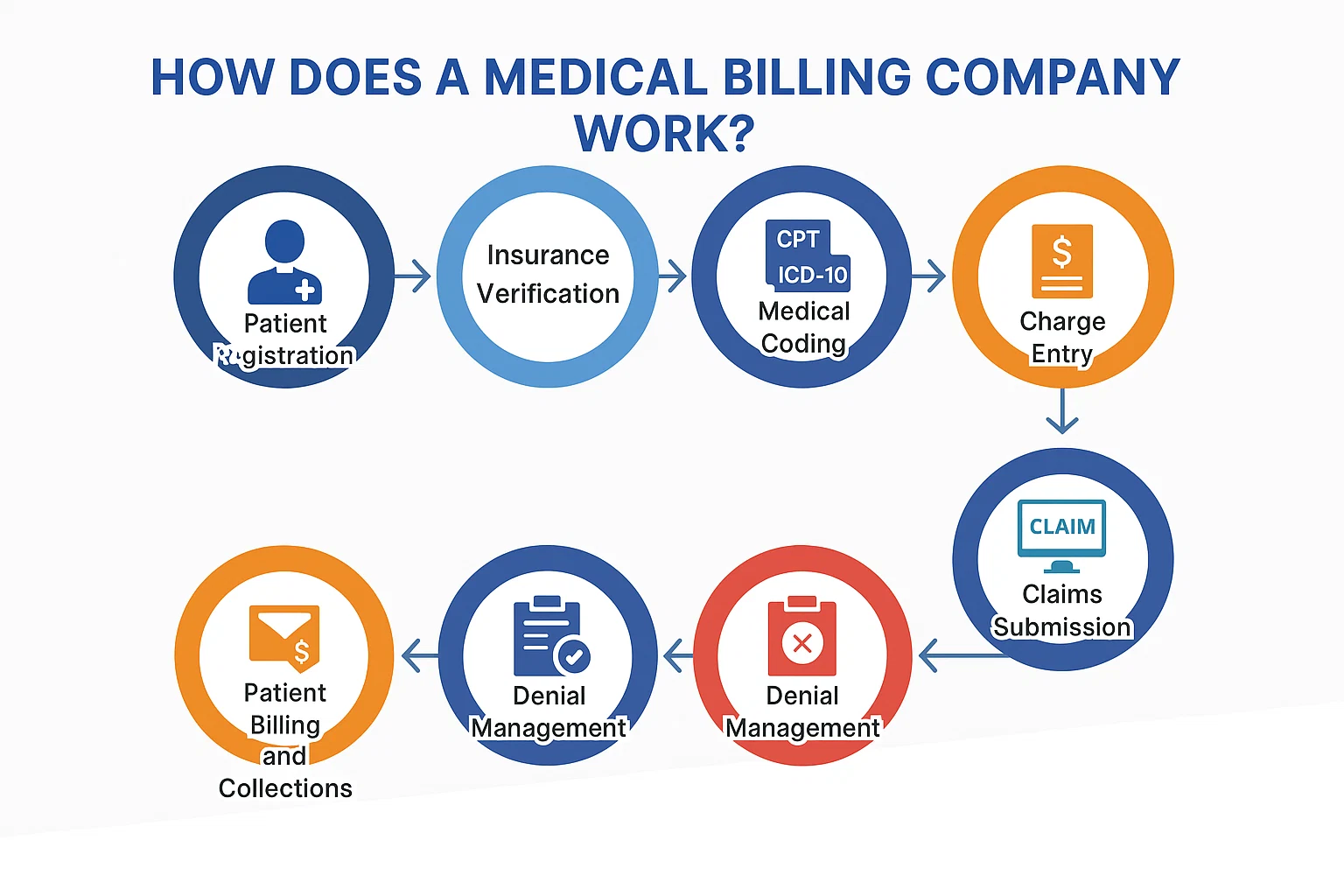
To fully understand the importance of medical billing in RCM, we need to look at the entire process, which includes the following key stages:
- Payment Posting and Patient Collections: Payments are posted once received from payers. Any remaining balance is billed to the patient. Prompt follow-ups help maintain consistent cash flow.
- Pre-registration and Insurance Verification: Before a patient visits, their demographic information and insurance details are collected. Accurate verification ensures that the services provided will be covered and paid for by the payer.
- Patient Registration: On the day of the visit, further information is collected, including patient consent, updated insurance details, and medical history. Errors here can lead to denied claims later.
- Medical Coding
- After the patient receives care, the procedures and diagnoses are translated into standardised codes (ICD, CPT, HCPCS). These codes are vital for the billing process.
- Medical Billing (Claim Generation and Submission): The medical billing team uses the codes to generate and submit claims to insurance companies. This step is crucial to getting reimbursed. Errors in billing can delay payments or lead to denials.
- Claim Management and Denial Handling: Claims are reviewed by payers and may be accepted, denied, or rejected. The billing team must follow up on denials, resubmit corrected claims, and ensure payment.
3. Medical Billing: The Heart of RCM
Medical billing sits at the heart of this entire process. Without a solid billing team or outsourcing partner, even the best clinical care may not result in proper reimbursement.
Here’s why medical billing is so essential in the RCM cycle:
- Ensures Timely Claim Submission: Delays in billing mean delays in payment. Professional billing services have systems to process and submit claims promptly, reducing the chance of late submissions or missed deadlines.
- Improves Claim Accuracy: Coding errors, patient information mistakes, or mismatched data can result in rejections. A strong billing process ensures accuracy from the start, lowering denial rates.
- Speeds Up Denial Management: Denied or rejected claims are inevitable. A competent billing team quickly identifies the issue, makes corrections, and resubmits, minimizing revenue loss.
- Optimizes Revenue Collection: Efficient billing processes maximize revenue by reducing unpaid claims, increasing patient collections, and enhancing reimbursement rates.
- Compliance with Regulations: Medical billing teams stay up-to-date with payer policies, coding updates, and regulatory changes (like HIPAA or ICD updates), keeping your practice compliant and audit-ready.
4. How Inefficient Billing Affects the Revenue Cycle
When billing is done poorly, it affects every aspect of the revenue cycle:
- Delayed Payments lead to cash flow issues.
- Increased Denials require more time and resources to resolve.
- Compliance Risks may trigger audits and penalties.
- Higher Operational Costs result from manual rework, resubmissions, and appeals.
- Patient Dissatisfaction increases due to billing errors or surprise charges.
These issues can hurt your healthcare facility’s reputation and bottom line.
5. In-House vs. Outsourced Medical Billing
One key decision healthcare providers must make is whether to handle billing internally or outsource it to a third-party service. Outsourcing offers several advantages within the RCM framework:
| In-House Billing | Outsourced Billing |
|---|---|
| Requires full-time staff & training | Access to specialized experts |
| High overhead costs | Cost-effective |
| Prone to internal delays | Faster claim turnaround |
| Limited compliance knowledge | Regularly updated with regulations |
| Time-consuming for providers | Frees up staff to focus on patient care |
Outsourcing is particularly beneficial for small and mid-sized practices looking to streamline operations and enhance revenue performance.
6. Technology’s Role in Medical Billing and RCM
Modern billing systems are no longer just about manual data entry. They now integrate AI, machine learning, and automation to:
- Auto-correct common billing errors
- Predict claim denials
- Suggest better codes for reimbursement
- Provide real-time analytics
- Automate patient billing and reminders
The integration of Electronic Health Records (EHRs) with billing platforms ensures smoother workflows, fewer errors, and more informed billing decisions.
7. Key Performance Metrics in RCM
Tracking these metrics helps assess how effective your billing process is:
- Days in Accounts Receivable (A/R) – How long it takes to collect payment.
- First-Pass Resolution Rate – Claims paid on the first submission.
- Denial Rate – Percentage of claims denied by payers.
- Net Collection Rate – Actual revenue collected vs. expected revenue.
- Patient Collection Rate – How much is collected from patients post-insurance.
Medical billing professionals use these metrics to refine the process and improve financial outcomes.
Conclusion
Medical billing isn’t just about sending invoices. It’s the financial engine that powers the entire healthcare revenue cycle. A robust billing system reduces denials, accelerates payments, and ensures compliance—directly impacting your organization’s financial stability.
Healthcare providers who prioritize professional, accurate billing—whether in-house or through outsourcing—position themselves for long-term success. In an era where profit margins are slim and regulations are tight, effective RCM supported by strong billing practices is not just smart—it’s essential.